Bile duct cancer, or intrahepatic cholangiocarcinoma in doctor-speak, is the deadliest of the liver cancers. Bile duct cancer is very hard to diagnose, and treatments so far have had varied success levels. Due to the location of the tumors, they can be nearly impossible to completely remove via surgery, and chemotherapy doesn’t always work. The survival rate of patients diagnosed with this kind of cancer is less than 5%.
How can we improve this situation? One option is to try to find a way to predict the outcome of individual patients so they can receive the best treatment. This is what Zeyuan Qiang and the rest of his team at Henan University set out to do. They hypothesized that how much of certain proteins in a patient’s cells, called biomarkers, could predict the survival and tumor characteristics of that specific patient.
Biomarkers are molecules in the body that can be measured to determine if an individual is healthy or not. A well-known example would be your blood pressure; doctors know that if your blood pressure is unnaturally high or low, there’s usually something wrong. The researchers of this study wanted to figure out if similar biomarkers could be used to detect bile duct cancer risk.
These proteins usually indicate cell division, which is important for detecting cancer which is a disease of uncontrolled cell division. The proteins chosen for this study were called AFP, CEA, CD10, CD34, and Ki67 (these are abbreviations for much longer names). The researchers hypothesized that variation in the levels of these five proteins could be used to determine the outcome of that patient’s disease, such as if their specific tumors are more likely to spread or if the patient’s overall chance of survival is very low.
Some of these proteins have been studied before to determine if they are biomarkers for other cancers. Ki67 was identified in 1983 as a sign of rapid cell division. Cancer is a disease of uncontrollable cell division, and this protein is an indicator if this is happening within the body. Because of this, the researchers believed that Ki67 would be a good biomarker for bile duct cancer.
The researchers chose archived tumor samples from 92 previous patients of bile duct cancer that didn’t go through chemotherapy or other treatments before surgery, had tumors partially removed, and did not have any infections after surgery. They followed up with these patients to gain some more information about their specific cases, such as treatment and recurrence of the cancer. These are important characteristics to know when determining things such as survival and
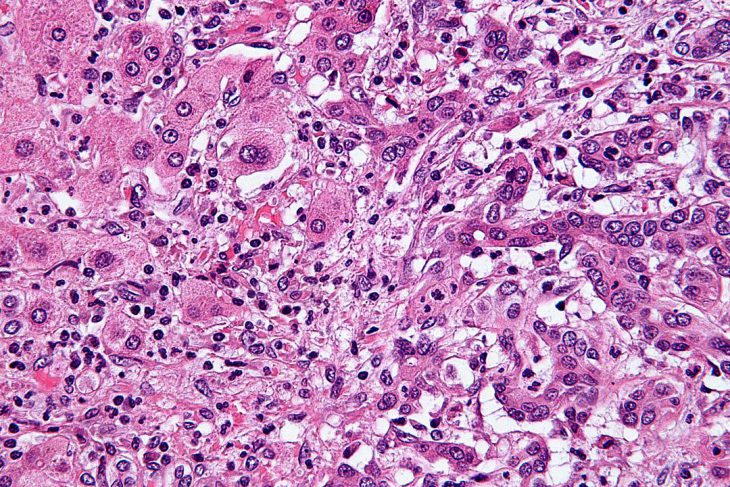
The researchers used a set of techniques called immunohistochemistry to visualize body tissues microscopically. The samples chosen were mixed with antibodies that had “tags” for each individual protein being studied. Antibodies are attracted to specific proteins in the body, so incubating the samples with these antibodies would allow them to bind to the desired proteins. Each protein was given a distinct antibody marker that turns brown if that protein is present. They viewed the stained, antibody-tagged samples under a light microscope and counted the number of cancerous cells in each sample.

This is the kind of image that is generated by the technique used in the study. The glowing spots show the antibody “tags.” Image by Emmanuelm via Wikimedia Commons (Creative Commons)
A score for the tumors was also given based on the intensity of the staining on the cells. A darker, more intense stain indicated a larger amount of the target protein. The samples were split into groups based on high or low scores. They then used statistical analysis to determine if the samples with certain levels of the biomarker proteins were statistically different from each other.
The results of this study showed that Ki67 as well as AFP and CEA (two of the other biomarkers considered) can indeed be used as a biomarker for bile duct cancer. They showed that higher levels of these proteins in cells usually meant larger tumor sizes, faster tumor metastasis, or spread, lower chance of survival with remission, and lower overall survival.
Knowing this information is crucial for choosing the best treatment for bile duct cancer patients because it tells practitioners how the tumor might respond. It may also predict how successful surgery would be for a particular patient, such as whether the tumor will regrow. The authors encourage other scientists to continue this research in larger groups of patients.